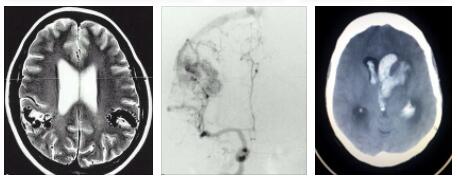
Bonnet-Dechaume-Blanc syndrome is the name of a very rare disease that is already congenital. The condition becomes noticeable through arteriovenous malformations on the retinal blood vessels and through changes in the face.
What is Bonnet-Dechaume-Blanc Syndrome?
In medicine, the Bonnet-Dechaume-Blanc syndrome is also known under the names congenital retinocephalofacial vascular malformation syndrome (CRC syndrome) or Wyburn-Mason syndrome. The French ophthalmologist Paul Bonnet (1884-1959) served as the namesake.
According to homethodology, Bonnet-Dechaume-Blanc syndrome is congenital and extremely rare. It is caused by a developmental disorder that occurs during embryogenesis. Typical features of the syndrome include unilateral arterviovenous malformations (malformations) on the retinal blood vessels of the eye, malformations of the cerebral and head blood vessels and changes in the face.
So far, many medical professionals have found it difficult to classify the Bonnet-Dechaume-Blanc syndrome precisely. It is not uncommon for the disease to be classified as a neurocutaneous syndrome. The rare Bonnet-Dechaume-Blanc syndrome has been known since the 19th century. Partial aspects were described by the German neuropathologist Hugo Spatz (1888-1969).
The first detailed case reports were made in the 1930s. The name Bonnet-Dechaume-Blanc syndrome came about in 1937 through a case report by the French doctors Paul Bonnet, Jean Dechaume and Emile Blanc. From 1943 came a case report by Roger Wyburn-Mason, so that this was also used as the namesake for the syndrome.
How many people suffer from Bonnet-Dechaume-Blanc syndrome could not be precisely determined. By 2009 there were 132 known cases of the disease. The syndrome shows up equally in both sexes.
Causes
The reason for the development of the Bonnet-Dechaume-Blanc syndrome is a developmental disorder during the 7th week of pregnancy. However, what causes this disorder is still unknown. The arteriovenous malformations (AVM) represent shunts that occur between the venous and arterial vasculature.
The vessels are often laid out in the form of a tangle and form a connection between the high and low pressure systems. Pressure increases blood flow to the vessels and causes them to expand. A continuous remodeling of the vascular bed takes place. Since this affects the vessel wall, complications such as narrowing and tearing of the vessels result.
Symptoms, ailments & signs
The Bonnet-Dechaume-Blanc syndrome is noticeable through various changes in the face, eyes and intracranial blood vessels, which depend on the form of the syndrome. In the case of a complete syndrome, in addition to the arteriovenous malformations of the retina and the cerebral vessels, there are also unilateral changes in the face.
These are mostly forehead, cheek or conjunctival vessels, some of which protrude. In addition, the eyelid vessels change. Sometimes the nose, ears or lips are also affected. Changes to the eyes occur with incomplete Bonnet-Dechaume-Blanc syndrome and isolated malformations of the retina. Almost 50 percent of all patients go blind on the affected side of the body.
There is also a risk of optic atrophy (loss of optic nerve cells) and secondary glaucoma. Also bleeding in the vitreous or the retina occur occasionally. A cerebral arteriovenous malformation can lead to outward strabismus (extropia), nystagma or ocular totality disorders.
Around two thirds of patients have arteriovenous malformations within the eye socket. In addition to cerebral malformations of the vessels, one-sided protrusion of an eyeball from the eye socket is possible. It is not uncommon for the optic nerve to be affected.
In the case of complete or incomplete Bonnet-Dechaume-Blanc syndrome, malformations of the cerebral vessels appear, which are primarily located in the supply region of the middle cerebral artery (arteria cerebri media). One third of the patients suffer from altered vessels in the cerebral segment of the visual pathway.
In some cases, the vascular changes do not cause any symptoms. In contrast, other patients are at risk of various forms of cerebral haemorrhage, increased intracranial pressure or symptomatic epilepsy. Paralysis of the facial nerve (facial paresis) is also possible.
diagnosis
If Bonnet-Dechaume-Blanc syndrome is suspected, the attending physician will conduct a neurological examination. Ophthalmological examination procedures such as perimetry (field of view measurement) or ophthalmoscopy (ophthalmoscopy) are also important. In order to visualize an arteriovenous malformation, a digital subtraction angiography, a computed tomography (CT) or a magnetic resonance tomography (MRT) can be carried out.
Magnetic resonance imaging is considered the best examination method, as it provides most of the data on the extent of the disease. The course of Bonnet-Dechaume-Blanc syndrome depends on the extent of the damage and on which part of the body it occurs.
Complications
Characteristic for the Bonnet-Dechaume-Blanc syndrome are pronounced malformations of the face, the blood vessels in the brain and the eyes. If the patient suffers from the complete syndrome, malformations of the eye retina and the cerebral vessels as well as unilateral facial changes are classic symptoms.
In many cases, the conjunctival, cheek and frontal vessels protrude. Other complications are changes in the eyelid vessels. The noses, ears, and lips can also be affected by this developmental disorder. The characteristic eye changes occur in the incomplete Bonnet-Dechaume-Blanc syndrome and in isolated malformations of the retina.
Every second patient goes blind on the affected side of the body. Further complications are the loss of optic nerve cells and secondary glaucoma. Bleeding in the retina or in the vitreous humor are potential side effects. Malformed blood vessels in the brain can lead to various forms of squint and the one-sided protrusion of the eyeball from the eye socket.
The malformed cerebral vessels are predominantly located in the supply area of the middle cerebral artery. Two thirds of patients have changes in the blood vessels within the eye sockets, often affecting the optic nerve. The cerebral segment of the visual pathway can also be involved.
Some patients do not notice any symptoms, while others develop complications such as increased intracranial pressure, cerebral haemorrhage, paralysis of the facial nerve or symptomatic epilepsy. The success of the treatment and the prognosis depend on the extent of the disease and the parts of the body involved.
When should you go to the doctor?
In most cases, Bonnet-Dechaume-Blanc syndrome is diagnosed immediately after birth or in the first few months after birth, so a visit to the doctor for diagnosis is not necessary. Those affected suffer from various changes and malformations, which mainly occur in the face of the affected person. However, it cannot be predicted how severely affected the person will be affected by this syndrome. In many cases, patients rely on various treatments that can make everyday life easier.
A doctor must be consulted, especially in the case of epileptic seizures caused by Bonnet-Dechaume-Blanc syndrome. However, paralysis of the face or cerebral haemorrhage can also occur as the disease progresses. Here, too, a visit to a doctor is absolutely necessary, as otherwise, in the worst case, the person concerned can die.
Usually, Bonnet-Dechaume-Blanc syndrome is diagnosed directly by a general practitioner or by a pediatrician. The further treatment of the syndrome is then carried out by the respective specialists. As a rule, not all complaints can be completely limited. Bonnet-Dechaume-Blanc syndrome may also reduce the patient’s life expectancy.
Treatment & Therapy
Treatment of Bonnet-Dechaume-Blanc syndrome should be carried out by a specialist in vascular anomalies in the case of arteriovenous malformation. However, therapy is rarely considered appropriate in babies or children. While treatment is not recommended for silent arterial lesions, intracranial impairment can be treated with embolization or proton beams.
If the malformations show up in other areas of the body, embolization is possible, which is followed by an operation. However, there is also the option of embolization alone or a single surgical procedure. As part of the embolization, the supplying vessels are closed.
Surgery cannot be performed on some patients. In such cases only embolizations take place. The neuroradiological surgeon glues the arteriovenous shunts together. For this purpose, he uses a catheter as part of an arteriography. However, there is a risk of skin necrosis with this procedure. In the case of a diffuse AVM, treatment with medication is an alternative.
Outlook & forecast
The prospect of a cure for Bonnet-Dechaume-Blanc syndrome is almost hopeless. The disease, with all its accompanying symptoms, represents a considerable burden for the patient throughout life. Therapy and medical care are made more difficult by the uncertainty of the cause. To this day, researchers and scientists have not been able to sufficiently substantiate the reasons for the developmental disorder. Therefore, the Bonnet-Dechaume-Blanc syndrome is treated according to the individual symptoms and complaints.
Refusing medical care is fraught with numerous complications and should be avoided. The deformations of the face and also the visual disturbance reduce the general well-being and the quality of life to a considerable extent. If cerebral hemorrhage sets in, the patient can also die.
Conventional medicine offers the patient opportunities to improve their health in a comprehensive treatment plan. The serious sequelae of Bonnet-Dechaume-Blanc syndrome are treated gradually and according to urgency. The additional complications from surgical interventions further worsen the prognosis.
Nevertheless, if the vascular changes are corrected, the patient can experience an alleviation of his symptoms. In addition to the current treatment, the treatment plan also includes further preventive examinations. These are intended to enable early detection of possible critical conditions in the patient in order to treat possible bleeding or increased intracranial pressure in good time.
Prevention
There are no preventive measures against Bonnet-Dechaume-Blanc syndrome. The triggering causes of the congenital malformations have so far remained unclear.
You can do that yourself
The cause of Bonnet-Dechaume-Blanc syndrome cannot be treated. The therapy focuses on surgical interventions and physiotherapy measures as well as cognitive training, whereby the therapy measures can be supported at home.
Parents of affected children should start cognitive training at an early stage and discuss this with the responsible specialist. The physiotherapeutic measures can be supported by moderate exercise. Depending on the age of the child, swimming, walking or targeted muscle training are ideal.
Since the Bonnet-Dechaume-Blanc syndrome can occur in a wide variety of types and forms, the measures must first be planned by a doctor so that a targeted improvement in the child’s state of health can take place. A change in diet is also an option. For example, avoiding certain foods can reduce the risk of epileptic seizures.
Finally, parents should watch their child carefully as there is an increased risk of accidents. In the event of a fall, the emergency services must be called. Failure to do so could result in serious complications such as vitreous or intraocular bleeding. Comprehensive therapeutic support is always required in addition to the measures mentioned.