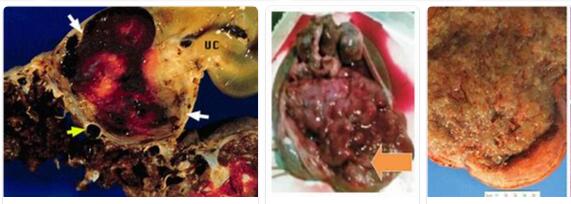
A malignant tumor in the trophoblast tissue is called chorionic carcinoma. This leads to rapidly progressing metastases.
What is chorionic cancer?
In medicine, chorionic carcinoma is also known as chorionic epithelioma, trophoblast tumor or villus cancer. What is meant is an infiltratively growing malignant tumor on the placenta consisting of anaplastic trophoblast cells. It occurs predominantly in women of childbearing age and is often the result of a mole of the bladder (mola hydatiosa).
The Latin term mole stands for the malformation of an embryo. In some cases, the tumor also occurs after an ectopic pregnancy, normal pregnancy, or miscarriage. Because chorionic carcinoma is considered an extremely aggressive tumor, rapidly growing daughter tumors (metastases) will soon develop. A seldom occurring variant is the non-gestational chorionic carcinoma of the ovary (ovary). This germ cell tumor often shows up in childhood or adolescence.
In Europe and the United States, the ratio of births to chorionic cancer is approximately 1 in 45,000. It is not uncommon for chorionic epithelioma to appear after the first pregnancy in women who are older than 30 years. Occasionally chorionic carcinoma can also be seen in males, where it occurs in the testes.
Causes
Often a chorionic carcinoma is the result of a mole of the bladder. In around 50 percent of all women affected, a mole developed in the run-up to the tumor. Another 25 percent suffered a miscarriage. For the remaining 25 percent, pregnancy was normal.
A mole appears only rarely. In most cases it is caused by faulty egg cell fertilization, after which there is no longer any genetic material. This leads to the degeneration of the placental villi into hundreds of vesicles, which explains the name of the mole. Because the small amniotic sac can no longer be adequately nourished, this causes it to perish.
The mole of the bladder is a benign trophoblastic disease caused by pregnancy. A DNA-less egg cell is fertilized by two sperm, which does not result in embryonic tissue, but only trophoblast tissue. Development from embryonic tissue and trophoblast tissue is also possible, which is referred to as incomplete molars.
Around two to three percent of all moles result in a malignant growth, from which the chorionic carcinoma emerges. The probability of degeneration fluctuates between 2 and 17 percent. Another conceivable cause of villus cancer is an increased immune tolerance to the father’s antigens.
A typical feature of chorionic carcinoma is the excessive production of the peptide hormone beta-hCG (human chorionic gonadotropin). For this reason, after successful treatment of the tumor, the beta-hCG levels in the blood are checked regularly.
Symptoms, ailments & signs
In the case of a mole of bladder, the abdomen grows rapidly. In more than two thirds of all women affected, the uterus is larger than the gestational age. Bleeding also occurs from the 11th week of pregnancy. In addition, labor-like pain and the loss of foamy, blistered fluid are recorded.
The main symptoms of chorionic cancer are vaginal bleeding, which occurs regardless of the menstrual cycle. If metastases already occur, this also results in various complaints. Depending on the degree of tumor growth and the occurrence of daughter tumors, it is important to differentiate between several stages.
These include non-metastatic chorionic carcinoma, destructive mole, metastatic chorionic epithelioma with low risk and metastatic chorionic epithelioma with high risk. We speak of high risk when metastases occur in the central nervous system, liver, lungs or pelvis.
Diagnosis & course
If a mole is suspected, a medical examination must be carried out. The pregnant woman’s uterus is palpated by the doctor. A typical feature is that the organ is too large for the respective stage of pregnancy. A sonography (ultrasound examination) reveals a snowy image instead of the heartbeat of the embryo.
Laboratory examinations are also important for diagnosing chorionic carcinoma. They can be used to determine increased beta-hCG levels. Another possible indication of the tumor is an increased concentration of alpha-1 fetoprotein (AFP), which is a glycoprotein that is only formed during pregnancy.
The combination of too large a uterus, ultrasound snowstorms and greatly increased beta-hCG levels in the urine or blood of women are reliable indicators of the presence of a trophoblast tumor. Chorionic carcinoma is one of the most aggressive tumors. Without rapid treatment, there is a risk of bleeding and haematogenous metastases in the vagina, liver, kidneys, lungs and brain. In principle, however, the prognosis for chorionic epithelioma is considered to be favorable, even if there is already metastasis.
Complications
Choriocarcinoma can cause a number of serious complications. First of all, there is a risk that the tumor will spread metastases to the vagina, kidney, liver, lungs and brain. This can lead to life-threatening bleeding, nerve disorders, pressure pain and other complications in the further course.
When a blood vessel is compressed, it can cause tissue death, blockage, biliary retention, or jaundice. Corresponding symptoms are associated with various secondary symptoms and can sometimes lead to permanent organ damage and death of the patient. If the chorionic carcinoma spreads into the brain, irreversible brain damage can occur.
In general, a malignant tumor in the trophoblast tissue increases the risk of circulatory disorders and thrombosis. If the tumor spreads to the gastrointestinal tract, further local complications can arise. There is a risk that a metastasis will break through the intestinal wall or cause inflammation of the peritoneum.
Another typical complication are fistulas, which arise mainly in the area of the urinary bladder and the uterus and can lead to infections and inflammations. With the treatment itself, serious complications are unlikely. Risks arise here from the chemotherapy itself as well as from the side effects of the drugs used.
When should you go to the doctor?
Since chorionic carcinoma usually leads to the formation of metastases relatively quickly, this tumor should be diagnosed and treated very early on. This can significantly increase the life expectancy of the person affected. As a rule, the doctor should be consulted if the patient’s abdominal volume has increased significantly without any particular changes having taken place in everyday life. Bleeding during pregnancy can also indicate chorionic carcinoma and should definitely be examined.
These also occur outside of the menstrual cycle. If the chorionic carcinoma is detected late, this can also lead to complaints in other regions of the body if the metastases have spread. For this reason, regular checkups during pregnancy are extremely important.
Diagnosis and treatment of this disease is usually carried out by a gynecologist. The removal of the tumor and the chemotherapy, however, require an inpatient stay in a hospital. Whether there will be a complete healing cannot be universally predicted.
Treatment & Therapy
A chorionic carcinoma is first treated surgically by scraping the uterus. Another scraping (curettage) may be necessary after four to six weeks to ensure that no diseased tissue remains. The next step in therapy is chemotherapy, during which methotrexate is administered.
In a mole of bladder, methotrexate has the property of shedding the contents of the uterus. In the case of chorionic epithelioma, the tumor responds well to the active ingredient. Healing is possible even in the early stages of metastasis. In later pregnancies, the risk of developing more moles is considered to be low. Follow-up care also plays an important role in therapy. Regular control of the hCG level is therefore necessary.
Outlook & forecast
With an early diagnosis and a quick start of treatment, chorionic carcinoma has a good prospect of a cure. Treatment is carried out by scraping the uterus in women and surgery in men. Depending on the severity and severity of the chorionic carcinoma, as well as the subsequent follow-up care, the patient is usually symptom-free and completely cured within a few weeks.
However, chorionic carcinoma has a very rapid disease process in men and women due to the strong growth. Without medical treatment, further metastases develop in the organism within a short period of time. These can affect the kidneys, liver, lungs or brain. In these cases, the chance of recovery drops significantly and the prognosis worsens considerably. If left untreated, those affected with chorionic carcinoma are therefore at risk of death and the disease is fatal.
In existing pregnancies, chorionic carcinoma causes a miscarriage in 25% of cases. The risk of developing a new chorionic carcinoma with another pregnancy is very low. However, if a miscarriage is experienced, there is an increased risk of secondary diseases appearing. Mental disorders are possible due to the loss of the unborn child. The vulnerability to depression, anxiety or sexual disorder is therefore increased by the disease.
Prevention
There are no known preventive measures against chorionic cancer. In the case of a molar bladder, a medical check-up should be carried out.
Aftercare
After successful treatment of chorionic carcinoma, the person affected must strictly adhere to the scheduled follow-up examinations. In any case, it is necessary to pay attention to contraception, since in the first year there is a risk of perforation of the placenta and at the same time the risk of miscarriage is increased.
In the case of metastatic tumors, monthly HCG controls are carried out in the first year. In addition, vaginal examinations should be carried out every four months and a CT examination of the thorax after about six months. The latter serves to rule out any lung metastases that may be present.
If the HCG value remains negative after this year, further HCG check-ups are only required as part of the vaginal examination and thus every four months for the next two years. The patient may also consider pregnancy in consultation with the attending physician.
If there are no increased HCG levels after this time, six-monthly checks are sufficient for a further two years to rule out a relapse. Affected people whose values are stable 5 years after the onset of the disease are recommended to have an annual check carried out for a further 5 years.
If a non-metastatic tumor was present, its location will determine further follow-up care. In general, however, no imaging is required here and the HCG controls are carried out at longer intervals. Patients may be able to consider pregnancy after six months.
You can do that yourself
A chorionic carcinoma is first treated surgically. After the procedure, the patient has to rest for a few days to weeks. If symptoms persist, a doctor’s visit is indicated. The doctor must perform a comprehensive physical examination after four to six weeks at the latest in order to ensure a smooth healing process.
If metastases have already formed, chemotherapy is indicated. Those affected are advised to talk to a specialist, as chemotherapy is always associated with certain risks. Accompanying this, precautionary measures must be taken for the start of treatment. Often the diet has to be changed, and a further medical examination is necessary. During the therapy, the body and especially the immune system should not be subjected to additional stress. Those affected are allowed to do moderate sport, but should also incorporate sufficient rest periods into everyday life.
There is often a lack of appetite after treatment. Therefore, the diet has to be changed and possibly supplemented with food supplements. Often, essential oils help stimulate the appetite. After the chorionic cancer has been removed, the patient should speak to the gynecologist again. A comprehensive examination must be carried out to determine whether the disease has caused infertility or other health problems that require treatment.